GYNECOMASTIA
Gynecomastia
Gynecomastia refers to the benign growth of breast tissue in men. Studies have shown that one out of every three men has gynecomastia. Gynecomastia, which can be seen both in infancy and adolescence and in adulthood, usually develops as a result of changes in the hormone level. Although it is not a development that is harmful to health, it has the possibility of causing problems such as stress disorder or body dysphoria. Long-term gynecomastia usually requires surgical treatment.
What is gynecomastia?
Estrogen and testosterone hormones in men need to be in a certain balance. The enlargement of the breast tissue as a result of the disruption of this balance is called gynecomastia. Gynecomastia, which is a benign tissue growth, can occur in one breast or in both breasts.
What Causes Gynecomastia?
Gynecomastia based on hormonal irregularities is common. In such cases, irregular or unbalanced estrogen and testosterone hormones lead to the development of the disease. A decrease in the amount of testosterone or an increase in the amount of estrogen in the body creates gynecomastia.
Gynecomastia, which is seen in male babies due to estrogen passed from their mothers, usually disappears on its own within three weeks after birth. Spontaneous resolution of gynecomastia seen in adolescence may take between six months and two years. In adult males, gynecomastia most commonly occurs between the ages of 50 and 69.
Other factors that can cause gynecomastia:
- Pituitary gland failure
- Imbalance in the secretion of the adrenal glands
- Hyperthyroidism, also known as over-secretion of thyroid hormone
- Liver failure
- It can be listed as problems such as kidney failure.
Moreover:
- Anti-androgen drugs that inhibit prostate enlargement or are used in the treatment of prostate cancer,
- Sports food supplements and androgens called anabolic steroids,
- Some antiretroviral group drugs used for the treatment of AIDS,
- anxiety medications,
- Antidepressants included in the tricyclic group,
- calcium channel blockers and
- Ulcer drugs have the possibility of causing gynecomastia.
What are the Symptoms of Gynecomastia?
- swelling in the breasts,
- extreme sensitivity,
- Ache,
- Fluid coming out of one or both breasts may be an indication of gynecomastia.
How is Gynecomastia Diagnosed?
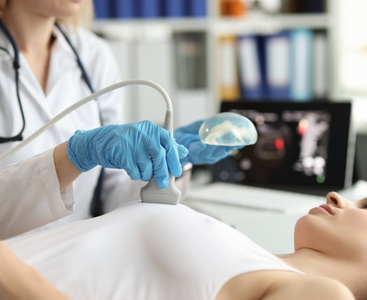
Manual examination is important for diagnosing gynecomastia. At the same time, patients are examined by imaging with ultrasound. After manual examination and ultrasound, it is possible to plan the most appropriate treatment for the patients.
How is Gynecomastia Treated?
The most appropriate treatment plan for the patient is determined by the type of gynecomastia. The course and response to treatment of gynecomastia in adolescents is measured using the Nydick classification. In this measurement, the type of gynecomastia is related to the size of the glandular tissue disc located under the brown ring on the nipple called the aerola. In cases with a disc diameter less than 4 cm, it would be more appropriate to inform the patient and wait for the gynecomastia to go away on its own. If the patient’s complaint lasts longer than 4 years or if the clinical findings that disturb the patient increase, treatment is started. Surgical intervention is recommended in cases where the disc diameter is greater than 4-6 cm.
One of the effective methods in the treatment of gynecomastia is surgical intervention. As a result of the examinations made by plastic surgeons, it is revealed what kind of operation should be planned. If there is glandular type gynecomastia, it is focused on removing the hard breast tissue. For lipomatous gynecomastia, a surgical intervention focused on removing fat tissue called liposuction is planned. For mixed type gynecomastia, a surgical operation using both of the above applications is used. The order and duration of the applications vary according to the prevalence rate of the tissues.
What Should Be Considered After Gynecomastia Surgery?
The recovery process after gynecomastia surgery varies according to the applied intervention. It is possible to see redness and swelling in the area after the treatment. This condition develops due to surgical incisions and disappears over time.
The patient can take a shower on the 3rd day after the operation. Limiting arm and shoulder movements after surgery helps the healing process.